

PHOTO CREDIT: Mayo Clinic
News
-
Gerstner Philanthropies Awards $7.9 million to emergency assistance providers through the Helping Hands Program
 March 1, 2023
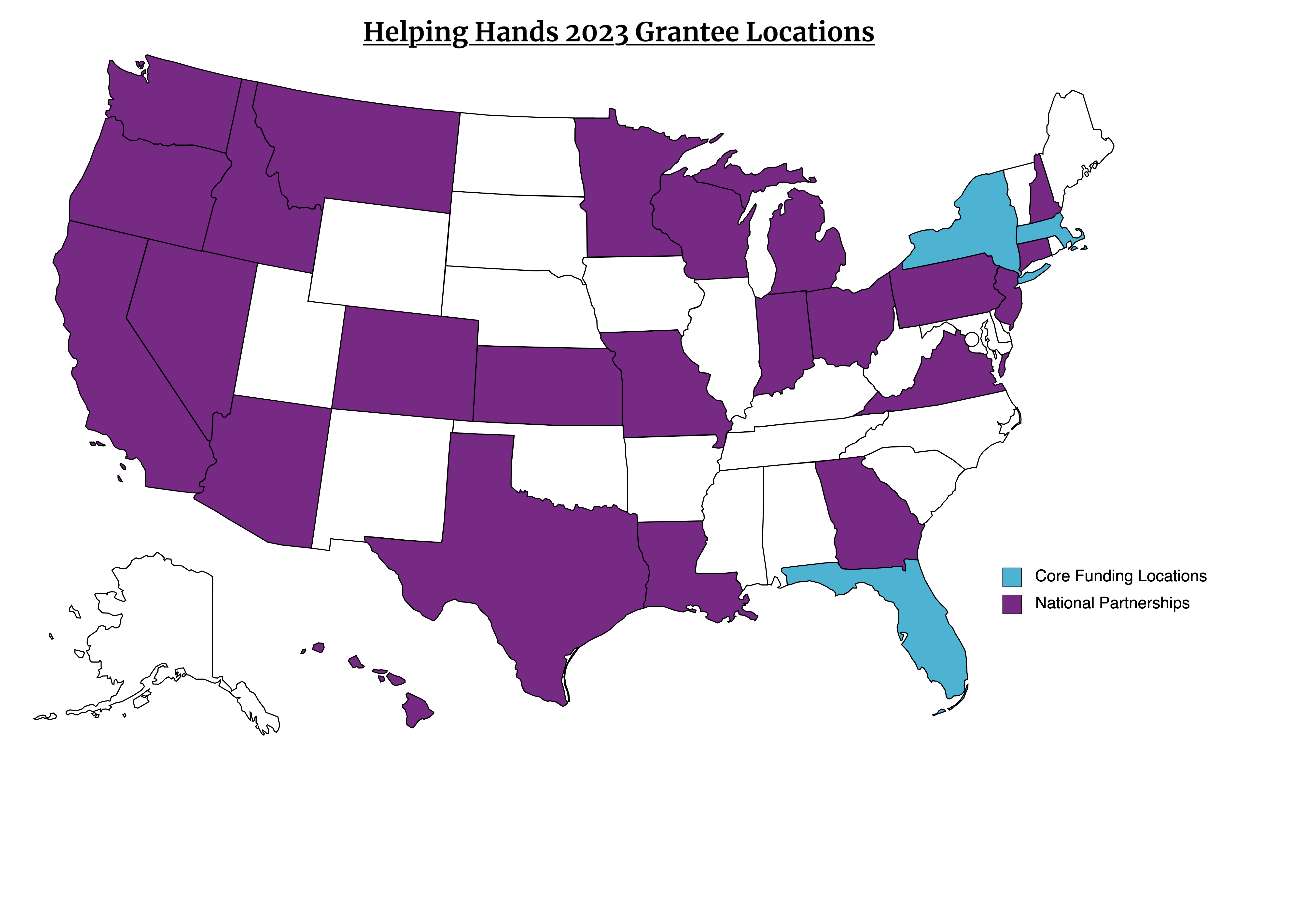
March 1, 2023As of March 1, 2023, Gerstner Philanthropies has awarded $7.9 million in Helping Hands funds to 24 social service organizations and colleges, a 47% increase from last year’s grantmaking. $7.3 million will expand support to existing emergency grant programs at 19 grantees across the country, with an additional $0.6 million supporting new partnerships with public colleges within the New York City area. Over $0.7 million of the awarded funds will support a new program capacity-building initiative at seven organizations with the goal of improving Helping Hands program efficiency and expanding its reach to serve more people in need.
Read the Full Press Release Here
-
Researchers at Columbia Invent Highly Accurate Sequencing Method to Study Cancer Tissues
January 20, 2023
Researchers at Columbia Engineering and Columbia University Irving Medical Center (CUIMC) have invented a new RNA sequencing method that achieves high-quality results from small volumes of frozen tumor specimens. They demonstrated the success of their technique in two clinical studies that profiled dozens of tumor samples, both those archived and those freshly collected, to understand how they respond to anti-tumor therapy.
Read the Full Article at newswise.com
-
Gerstner Scholar at AMNH Identifies Mechanism for Glass Frogs Unique Transparent Abilities
 December 23, 2022
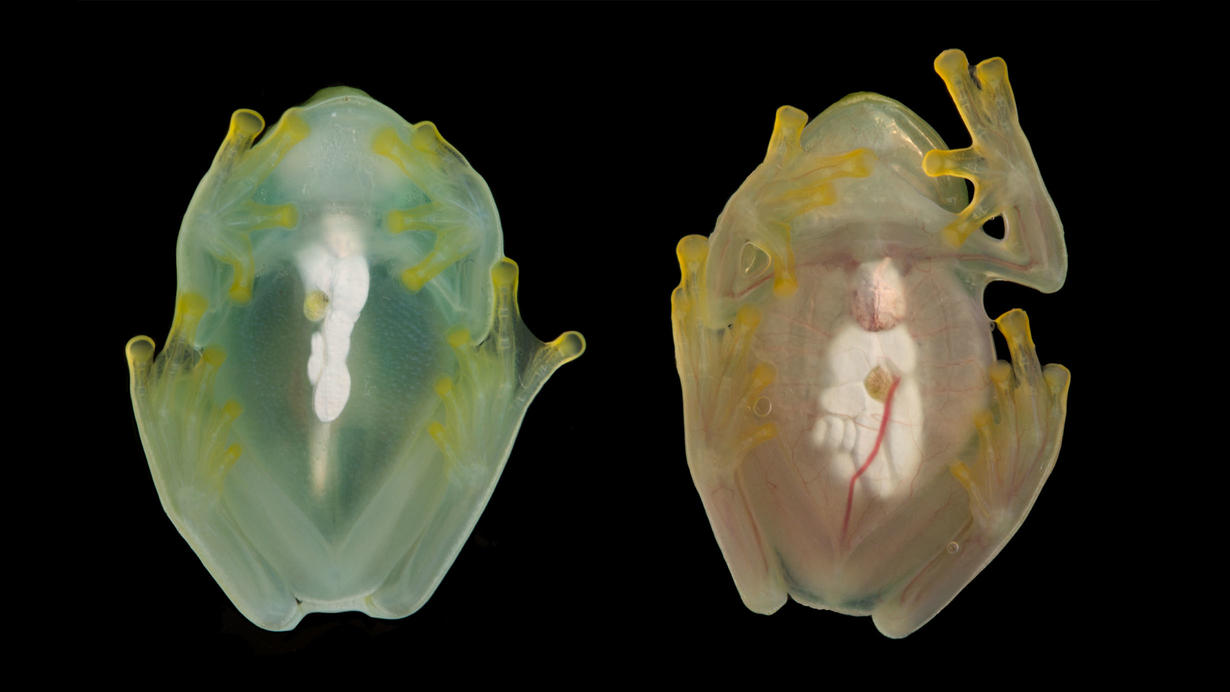
December 23, 2022A new study from Gerstner Scholar Jesse Delia and researchers at the AMNH identified the mechanism that allows Glass frogs to maintain their unique transparency. Researchers had previously observed Glass frogs shifting into a transparent state during rest periods as a means to camouflage themselves. By using soundwaves to identify where the Glass frogs were storing their red blood cells, Delia and his colleagues observed the Glass frogs storing up to 89% of their red blood cells within the liver. This ability, and the fact that the Glass frogs did not develop any bloods clots could have potentially large benefits for blood-clotting treatment in humans.
Read More at NYtimes.com
-
Gerstner Philanthropies Grants $950K in support of Hunger Prevention
 December 9, 2022
December 9, 2022Gerstner Philanthropies is excited to announce that it has awarded $950,000 to eight organizations across our core funding locations to support hunger prevention in our communities in 2023. These organizations provide food and related assistance to an increasing number of individuals and families struggling from the impacts of inflation and rising housing costs. These funds will be utilized by our grantees to continue to implement critical programs, such as mobile pantries and meal delivery for clients in food deserts, food rescue programs and one of the largest kosher and halal food pantries in the country. This announcement comes on the heels of three Thanksgiving meals grants totaling $43,200 to partners in Palm Beach, Boston, and Greater New York City, providing over 800 families with turkey dinners over the holidays.
Read the full list of food grants on our grants page
-
Gerstner Philanthropies Visits with Gerstner Scholars at John Carroll High School
 December 5, 2022
December 5, 2022This week, our Chairman, Louis V. Gerstner, Jr., and our Executive Director Kara Klein had the opportunity to meet with Gerstner Scholars at John Carroll High School in Fort Pierce, Florida. The Louis V. Gerstner, Jr. Distinguished Scholars Program was established in 2005. Since that time the foundation has invested over $4.7 million dollars to support scholarships at the three high schools within the Diocese of Palm Beach. The scholarship supports outstanding students with financial need. Principal Corey Heroux expressed her gratitude by sharing “It was such a gift for our Gerstner scholars to meet Mr. Gerstner and to hear from him so many beautiful pearls of wisdom about how to pursue success and to live a meaningful life marked by service to others.”

